Invasive care procedures and neonatal sepsis in newborns with very low birth weights: a retrospective descriptive study
Flávia do Valle Andrade Medeiros1, Valdecyr Herdy Alves1, Cristina Ortiz Sobrinho Valete1, Eny Dórea Paiva1, Diego Pereira Rodrigues1, Renata Rangel Birindiba de Souza1
1Fluminense Federal University
ABSTRACT
Aim: To identify the type of sepsis which affected newborns with very low birth weight and invasive care procedures to which they were subjected in a university hospital in the city of Niterói, between the years 2008 and 2012. Method: This is a retrospective descriptive study using secondary data research in the medical records of newborns admitted to the Neonatal Intensive Care Unit of the University Hospital Antônio Pedro. Results: Of the 49 infants studied, 35 were diagnosed with early sepsis, eight with early and late sepsis and six late. The mean gestational age was 30.5 weeks and the weight 1.176,1 kg. The most frequently performed care procedures were: peripheral venipuncture (87.8%), central catheter peripheral venipuncture (81.6%), assistance to ventilation in the delivery room (69.4%) and intubation in the delivery room (28.6%). Conclusion: It is inferred that the lower birth weight is associated with the higher incidence of sepsis.
Descriptors: Sepsis; Newborn; Intensive Care Units Neonatal; Nursing.
INTRODUCTION
Certain complications of extreme prematurity still remain as challenges to be overcome regarding the assistance to the newborn (NB) hospitalized in neonatal intensive care units (NICU)(1). Among other complications are the healthcare associated infections (HAIs), formerly known as nosocomial infections, especially bacterial, that determine the quality of hospitalization of these NBs and their survival(2) and, especially, the child mortality assessment(3) related to the HAIs in the NICU.
From 2013, the Agência Nacional de Vigilância Sanitária (Anvisa) (National Health Surveillance Agency) determined the HAIs definition criteria in neonatology, classifying them according to their origin, from three routes: trans-placental infections; early HAIs, possible maternal origin occurring up to 48 hours of life and late HAIs, hospital origin, manifested in newborns after 48 hours of life(1,4,5).
The approach of HAIs in this study concerns the understanding of the focus of the origin of the inflammatory process, since sepsis is defined as the systemic response to the infection syndrome characterized by the clinical evidence of the infection(1).
Sepsis and meningitis are the main responsible factors for morbidity and mortality in the neonatal period, affecting mainly the NBs with very low birth weights, namely those weighing less than 1,500 g, presenting immunological characteristics and immature and diminished barriers, favoring the development of infections(1).
More than 30% of newborns are affected by HAIs, while, in an older pediatric population, these rates can be up to five times smaller. In Brazil, over 60% of child deaths occur in the neonatal period, and sepsis is a major cause(4).
Neonatal sepsis is considered probable or clinical when the blood culture is negative and proven when presenting a positive blood culture. The presence of one or more signals that indicate three of the frameworks establish the criteria for clinical diagnosis of sepsis: apnea, bradypnea, grunting, tachypnea, sternal and subcostal retractions, nasal flaring and cyanosis; temperature instability (hypothermia <36,5º and hyperthermia> 37.5º); hypotonia and seizures; irritability and hypo-activity/lethargy; gastrointestinal symptoms such as abdominal distension, vomiting, gastric residue and difficulty with food intake; idiopathic jaundice; pallor, cold skin, excessive sweating, hypotension and capillary filling time exceeding three seconds; glucose intolerance; signs of bleeding with symptoms suggestive of disseminated intravascular coagulation; subjective assessment: NB that "does not look good"(4,5).
The low sensitivity of the test makes the diagnosis difficult and uncertain, especially in the early neonatal sepsis. When properly trained, the nursing team has a key role in the early diagnosis of sepsis, for it remains longer with the NB, allowing better observation(4). Since the neonatal sepsis occurs in 25% of premature and low birthweight infants at birth(6), it is necessary for the multi-professional team to ensure care in order to prevent it in the NICU and ensure the NBs’ survival and quality health care.
Delayed psychomotor development of babies born prematurely and affected by neonatal sepsis is the most significant consequence of damage to the brain tissue, promoted by the intense inflammatory response to infection(7).
Major challenges are becoming common in neonatology services: first, identify infants with a high probability of developing sepsis in order to initiate antibiotic therapy; second, distinguish healthy children, but who have a high risk of children with clinical signs that do not require treatment; and, third, stop using antibiotics since sepsis is considered unlikely(8).
Assistance to infants with very low birth weights requires the practice of care procedures that need attention and rigor from the special multidisciplinary team. Acceptance in terms of the risk of pre-term in the NICU is an event which demands complex, intense, invasive and necessary procedures, as they are valuable tools for assessing and maintaining the lives of these babies with very little chance of survival(1).
Based on ANVISA criteria, the cases of early HAIs without the maternal risk factor and NBs undergoing invasive procedures should be considered as probable nosocomial and should be classified as early hospital infection(4). Moreover, the late sepsis is set by bacterial invasion originated from the environment and is characterized as nosocomial and related to care(4). Thus, these infections were divided by ANVISA into location sites. Invasive care procedures are related to the following sites: primary infection of the bloodstream, infection related to health care of the respiratory tract, urinary tract infection and infection of the gastrointestinal system(4).
Often preterm NBs are subjected to procedures soon after birth, because of their need for early physiological care. Low birth weight NBs are extremely susceptible to hypoxia due to maternal, fetal and placental disease and often need procedures for immediate resuscitation after delivery(1). Mechanical ventilation, parental nutrition, the use of an orogastric catheter, antimicrobial therapy, the use of a central venous catheter and birth weight are factors that appear to be associated with increased risk of HAIs(9).
Almost 70% of deaths in the first year of life correspond to the neonatal period and are probably due to the lack of appropriate care for NBs. This is the great challenge – to reduce infant mortality in our country(10).
In this study, the quantified results sought an approach based on evidence of the dynamics of HAIs in NBs admitted to the NICU, aiming to facilitate a diagnosis of care practice and signal adjustments in carrying out invasive procedures in newborns in the NICU, as well as the approach to pregnant women in prenatal care, in order to control premature births and possible early sepsis occurrences.
Given the above, the purpose of the study was to identify the type of sepsis affecting infants with very low birth weight and the invasive care procedures to which they were submitted in a university hospital in the city of Niterói, between the years 2008 and 2012.
METHOD
This is a retrospective descriptive study, based on secondary data research, through systematized data collection from the medical records of infants with very low birth weights admitted to the NICU and in the epidemiological surveillance records at the Hospital Infection Control Commission (HICC) of the Hospital Universitário Antônio Pedro (HUAP) (Antonio Pedro University Hospital), Universidade Federal Fluminense (UFF) (Fluminense Federal University).
The study was submitted to the Research Ethics Committee of the HUAP, Fluminense Federal University, as provided for in Resolution 466/12 of the National Health Council, and approved under opinion No. 426,309/2013, with CAAE: 13565613.9.0000.5243.
The NICU at HUAP consists of seven beds and, between the years 2008 and 2012, there were a total of 486 hospitalizations, according to the records of the hospital management system of the institution. The study population consisted of all infants with very low birth weights (weighing between 1,000g - 1,500g) admitted during that period and recorded in the Nosocomial Infection Surveillance System (NISS) of the hospital CCIH diagnosed with neonatal sepsis, determining the sample size as forty-nine (49) NBs.
The NISS system was created in the United States in the 70s, by the Centers for Disease Control (CDC), aiming at the formation of a national database and voluntary reporting that would ensure the control of infections in the participating hospitals. From these data, the CDC has formulated a standard protocol for the classification of infections with clinical and laboratorial criteria. The surveillance covered adult and pediatric ICU, high-risk nursery and surgical patients(11).
The invasive care procedures selected for this study were: arterial and venous umbilical catheter, peripherally inserted central catheter (PICC), peripheral venous access, endotracheal intubation and bladder catheterization, selected according to the Infection Diagnostic Criteria Related to Health Care - Neonatology (Anvisa)(4), associated with the neonatal infection definitions for the following topographies: primary clinical bloodstream infections and confirmed microbiologically, respiratory tract HAIs, central nervous system infections, urinary tract infections and infections of the gastrointestinal system.
The construction of the database was made from information collected in the records and developments of the multidisciplinary team and the records of the surveillance data sheets when given access to the medical records of the NBs in the medical file.
The inclusion criteria of the patients studied were: weight between 1,000 and 1,500 g; registered in the NISS of the HICC for introducing neonatal sepsis; having been born in the period between 2008 and 2012 at the hospital where the study was conducted; having been subjected to invasive care procedures in the delivery room and/or in the NICU and having been admitted to the NICU immediately after delivery. The exclusion criteria were: NBs transferred from other hospitals or admitted to the Intermediate Unit or Rooming soon after delivery, without staying in the NICU.
Descriptive statistics were used with the averages and frequency of the explanatory variables related to the NBs, to the referred invasive care procedures and to the occurrence of sepsis. According to ANVISA, early neonatal sepsis was defined as one that occurs in the first 48 hours of life, related to maternal factors, pregnancy and peripartum; and late-sepsis as infectious processes manifested in NBs after 48 hours of life(4).
Infants were categorized into three groups according to the diagnosis of the type of sepsis that had developed: early, late or both. Data were entered into Microsoft Excel® version 2010 software and transferred to the Stata® version 6.0 (Stata Corp), where they were analyzed and presented in the form of tables and graphs.
RESULTS
Among the 49 medical records of infants with very low birth weight diagnosed with neonatal sepsis between 2008 and 2012, it was found that 71.4% (n=35) showed early sepsis, while 16.3% (n=8) presented early and late sepsis and 12.2% (n=6), late sepsis, as shown in Graph 1.
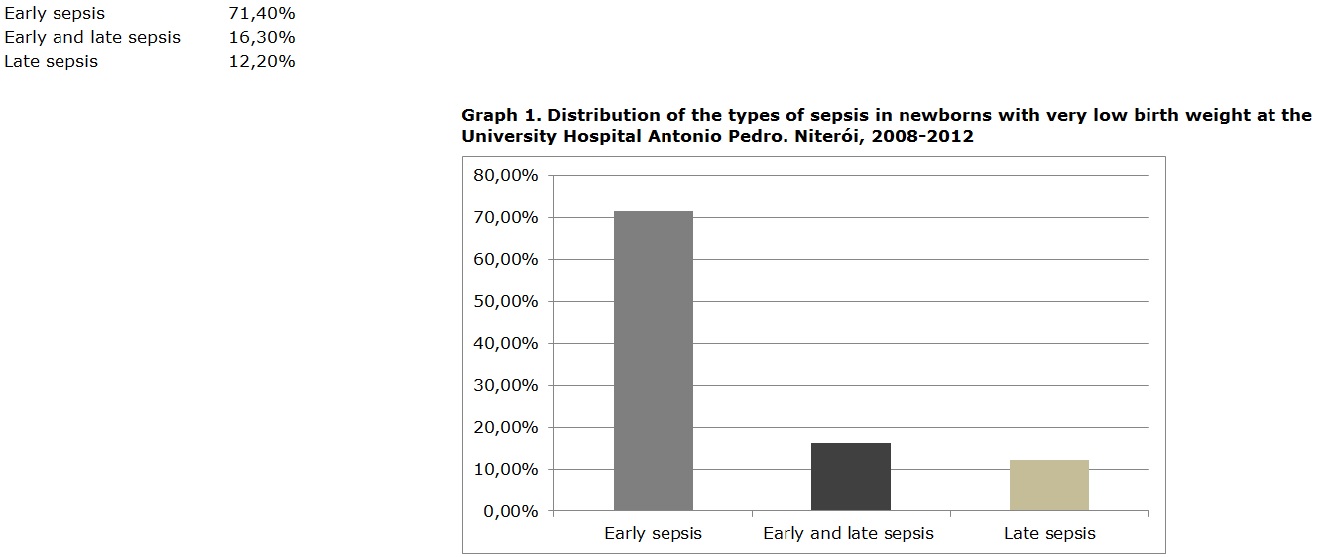
Table 1, below, describes the characteristics of the 49 NBs enrolled in the study, with their respective frequencies and means.

In the characterization of the NBs, the mean gestational age was 30.5 weeks and the average weight of 1.176,1 g. The most common gender was female and cesarean delivery was predominant at 75.5%. The frequency of deaths was 10.2%.
Given the small value of n of the late sepsis group and the group of both early and late sepsis, in Tables 1 and 2, they were redistributed into two groups: early sepsis group and the other groups with the characterization of the NBs and the occurrence of sepsis.

The mean gestational age in both groups was 30 weeks. The average weight in the early sepsis group was 1.160g, and in the group of other sepsis, 1.060g. The females (54.3% in the early and 57.1% in the other) and cesarean section (early 77.1% and 71.4% in the other groups) have prevailed.
Table 3 shows the care, invasive procedures performed and the occurrence of sepsis.

The peripheral venous access occurred in 87.8% (n=43) of the 49 NBs, in which 85.7% (n=30) were in the early sepsis group (n=35) and 85.7% (n=12) in the other sepsis group (n=14). On the other hand, the peripherally inserted central catheter was used in 81.6% (n=40) of cases, of which 74.3% (n=26) were in the early sepsis group (n=35) and 92.8% (n=13) were in the other sepsis group (n=14).
The aspiration of the upper airways occurred in 69.4% (n=34), of which 74.3% (n=26) were in the early sepsis group (n=35) and 57.1% (n=8) were in the other sepsis group (n=14). The orotracheal intubation was performed in the NICU in 36.7% (n=18) of the 49 NBs, including 31.4% (n=11) of the early sepsis group (n=35), and 50% (n=7) in the other sepsis group (n=14). In 28.6% (n=14) of the 49 NBs there was no need for intubation in the delivery room, of which 25.7% (n=9) were in the early sepsis group (n=35) and 35.7% (n=5) were in the other sepsis groups (n=14).
DISCUSSION
Early sepsis stood out for its major frequency in the NBs included in the study, all diagnosed only by the clinic, without bacterial growth in the collected cultures, which corroborates other studies that have also confirmed only the clinical diagnosis(12-14).
The low sensitivity and specificity of laboratory tests, most often inconclusive, limits the confirmation of results(10).
Despite being mentioned as one of the most common diagnoses made in the NICU(8), the high prevalence of early sepsis is a result that differs from that commonly found in the literature and in various studies in Brazil, where late-sepsis is usually associated with the environment and care procedures of hospital origin, besides being the most common in the NICU(9,13). In the literature, there is no epidemiological evidence to support the increased risk for late-sepsis followed by early sepsis in NBs surviving, compared to those who do not have the early sepsis, even requiring longer hospital stays, more days of parental nutrition and mechanical ventilation and increased risk of death. Interestingly, results suggest a possible slight reduction in the subsequent risk of late-sepsis in the early sepsis group, which deserves further study(15).
Considering the fact that the early sepsis group presented a greater number of cases in this study and the fact that its causes are associated with maternal conditions, low birth weight stood out as a factor related to NBs that offers risk of infection and can be associated with hypertensive disorders of pregnancy (HDP), noninfectious maternal factors, which, in the clinical course in pregnant women, cause the need for premature termination of the pregnancy. It is noteworthy that prematurity and low weight offer conditions for NBs to develop infections. Considering the characteristic conditions of prematurity and the need for care in the ICU, prematurity is the main risk factor for the development of sepsis in NBs(10).
The mean gestational age of the NBs included in this study was 30 weeks. This finding is similar to those of some other studies, in which gestational ages of 29-30 weeks have also prevailed(7,10). The mean birth weight was 1.176g, as observed in studies that focus on infants with very low birth weights(7,10,16). Although, according to the Ministry of Health(10), the male NB is twice as likely to develop early sepsis, in this study, females were the most frequent in both sepsis groups.
Regarding the exposure factors of NBs to the risk of infection among the risk procedures for primary bloodstream infection, the vascular access rates were the highest, as they were 88% for peripheral venous access and 81% for the central catheter peripherally inserted. In a study in an NICU in Tubarão, Santa Catarina, the HAIs rate was 45.8%, and it showed a higher frequency of peripheral venous access (43.8%)(14).
The use of PICC has already generated studies that demonstrate a significant length of time associated with infectious risk(17,18). Despite these findings, the PICC continues to be the long stay venous access, which is more appropriate for infants with very low birth weight, according to the recommendation of the Ministry of Health(10).
As for the respiratory tract, the most common were the aspiration of the upper airways (69.4%) and the orotracheal intubation in the NICU (36.7%) and in the delivery room (28.6%). Studies show percentages for the orotracheal intubation and the high risk that this procedure provides for pneumonia in NBs with very low weight(9,20).
The death rate among the infants studied was 10.2%, a result that is below the results shown in other studies on the HAIs and sepsis(20). According to the Ministry of Health, the mortality rate in preterm infants weighing less than 1,500 g is on average 25%(20).
Thus, it is increasingly urgent that the team adopts systematic practices in the management of infants with very low birth weights, making everyone accountable for the careful and accurate execution of the protocols and routines. An interesting way to achieve this systematization of assistance would be the construction and adoption of "bundles" of care, which would allow a more practical and objective form of care.
CONCLUSION
It can be concluded that, in the study group, the most frequent sepsis was the early one and it was not possible to identify the risk of late sepsis from it. The lower birth weight was associated with a higher frequency of sepsis other than just the early sepsis. The death rate was low. The vascular accesses were the most frequent invasive care procedures.
The limitations encountered during the development of this study were the absence of maternal data of prenatal care in the medical records of NBs and building renovation in the maternity unit and neonatal intensive care unit during the collection of study data, which caused a reduction in the number of hospitalizations and, consequently, the quantity of NBs.
Thus, better data on neonatal sepsis could contribute to changes in care practices, endorsed by protocols recommended for the reduction of sepsis in the Neonatal Intensive Care Unit, thus contributing significantly to the quality of care for NBs.
REFERENCES
- Aguiar CR, Costa HPF, Rugolo LMSS, Sadeck LSR, Costa MTZ, Pachi PR, et al. O recém-nascido de muito baixo peso 2a ed. São Paulo: Atheneu; 2010.
- Ministério da Saúde (Brasil). Atenção à saúde do recém-nascido: guia para profissionais de saúde. Volume 1. Brasília: Ministério da Saúde; 2011.
- Basso CG, Neves ET, Silveira A. The association between attending prenatal care and neonatal morbidity. Texto Contexto Enferm [internet]. 2012 [cited 2015 Jun 22]. 21(2): 269-76. Available from: http://www.scielo.br/pdf/tce/v21n2/en_a03v21n2.pdf http://www.scielo.br/pdf/tce/v21n2/en_a03v21n2.pdf
- Ministério da Saúde (Br). Critérios diagnósticos de infecções relacionadas à assistência à saúde neonatologia. Brasília: Ministério da Saúde; 2013.
- Silveira RC, Giacomini C, Procianoy RS. Neonatal sepsis and septic shock: concepts update and review. Rev. Bras. Ter. Intensiva [internet]. 2010 [cited 2015 Jun 22]. 22(3): 280-90. Available from: http://www.scielo.br/pdf/rbti/v22n3/en_11.pdf
- Migoto MT, Souza SNDH, Rossetto EG. Skin lesions of newborns in a neonatal unit: descriptive study. Online Braz J Nurs (Online) [Internet]. 2013 [cited 2015 Jun 22]. 12(2): 377-92. Available from: http://www.objnursing.uff.br/index.php/nursing/article/view/4042/pdf_1
- Hentges CR, Silveira RC, Procianoy RS, Carvalho CG, Filipouski GR, Fuentefria RN, et al. Association of late-onset neonatal sepsis with late neurodevelopment in the first two years of life of preterm infants with very low birth weight. J. Pediatr. (Rio J.) [internet] 2014 [cited 2015 Jun 22]. 90(1): 50-7. Available from: http://www.scielo.br/pdf/jped/v90n1/0021-7557-jped-90-01-00050.pdf
- Polin RA. Management of neonates with suspected or proven early-onset bacterial sepsis. Pedatrics [internet]. 2012 [cited 2015 Jun 22]. 129(5): 1006-17. Available from: http://pediatrics.aappublications.org/content/pediatrics/129/5/1006.full.pdf
- Brito DVD, Brito CS, Resende DS, Moreira do ÓJ, Abdallah VOS, Gotijo Filho PP. Nosocomial infection in Brazilian neonatal intensive care unit: a 4-years surveillance study. Rev. Soc. Bras. Med. Trop [internet]. 2010 [cited 2015 Jun 22]. 43(6): 633-37. Available from: http://www.scielo.br/pdf/rsbmt/v43n6/06.pdf
- Ministério da Saúde (Br). Atenção à saúde do recém-nascido: guia para profissionais de saúde. Volume 2. Brasília: Ministério da Saúde; 2011.
- Rangel R. Monitoramento de Infecções Relacionadas à Assistência à Saúde [homepage]. Rio de Janeiro; 2014. [cited 2015 Oct 22]. Available from: http://portal.anvisa.gov.br/wps/wcm/connect/5209fb8043ec44cfacd2ee6b7f09096f/Monitoramento+de+IRAS+-+Dra+Rosana+M+Rangel.pdf?MOD=AJPERES
- Chann GJ, Baqui AH, Modak JK, Murillo-Chaves A, Mahmud AA, Boyd TK, et al. Early-onset neonatal sepsis in Dhaka, Bangladesh: risk associated with maternal bacterial colonisation and chorioamnionitis. Trop Med Int Health [internet]. 2013 [cited 2015 Jun 22]. 18(9): 1057-64. Available from: http://www.ncbi.nlm.nih.gov/pubmed/23822861
- Ferreira J, Bouzada MCF, Jesus LA, Cortes MCW, Armond GA, Clemente WT, et al. Evaluation of national health-care related infection criteria for epidemiological surveillance in neonatology. J. Pediatr. (Rio J.) [internet]. 2014 [cited 2015 Jun 22]. 90(4): 389-95. Available from: http://www.scielo.br/pdf/jped/v90n4/0021-7557-jped-90-04-00389.pdf
- Dal-Bó K, Silva RM, Sakae TM. Nosocomial infections in a neonatal intensive care unit in South Brazil. Rev Bras Ter Intensiva [internet]. 2012 [cited 2015 Jun 22]. 24(4): 381-5. Available from: http://www.scielo.br/pdf/rbti/v24n4/en_a15v24n4.pdf
- Wunn JL, Hansen NI, Das A, Cotton M, Goldberg RN, Sánchez PJ, et al. Early sepsis does not increase the risk of late sepsis in very low birth weight neonates. . J. pediatr. (Rio J.) [internet]. 2013 [cited 2015 Jun 22]. 162(5): 942-8. Available from: http://www.ncbi.nlm.nih.gov/pubmed/23295144
- Figueiró-Filho EA, Oliveira VM, Ferreira CM, Silva VM, Tinos ALS, Kanomata LB. Variáveis perinatais e associação de recém-nascidos de muito baixo peso ao nascer em hospital público universitário do Brasil. Rev Bras Ginecol Obstet [internet]. 2014 [cited 2015 Jun 22]. 36(1): 10-6. Available from: http://www.scielo.br/pdf/rbgo/v36n1/0100-7203-rbgo-36-01-00010.pdf
- Sengupta A, Lehmann C, Diener-West M, Perl TM, Milstone AM. Catheter duration and risk of CLA-BSI in neonates with PICCs. Pediatrics [internet]. 2010 [cited 2015 Jun 22]. 125(4): 648-53. Available from: http://www.ncbi.nlm.nih.gov/pubmed/20231192
- Milstone AM, Reich NG, Advani S, Yuan G, Bryant K, Coffin SE, et al. Catheter dwell time and CLA-BSIs in neonates with PICCS: a multicenter cohort study. Pediatrics [internet]. 2013 [cited 2015 Jun 22]. 132(6): 1609-15. Available from: http://www.ncbi.nlm.nih.gov/pubmed/24218474
- Freitas BAC, Peloso M, Manella LD, Franceschini SCC, Longo GZ, Gomes AP, et al. Late-onset sepsis in preterm children in a neonatal intensive care unit: a three-year analysis. Rev. bras. ter. intensiva [internet]. 2012 [cited 2015 Jun 22]. 24(1): 79-85. Available from: http://www.scielo.br/pdf/rbti/v24n1/en_12.pdf
All authors participated in the phases of this publication in one or more of the following steps, in According to the recommendations of the International Committee of Medical Journal Editors (ICMJE, 2013): (a) substantial involvement in the planning or preparation of the manuscript or in the collection, analysis or interpretation of data; (b) preparation of the manuscript or conducting critical revision of intellectual content; (c) approval of the versión submitted of this manuscript. All authors declare for the appropriate purposes that the responsibilities related to all aspects of the manuscript submitted to OBJN are yours. They ensure that issues related to the accuracy or integrity of any part of the article were properly investigated and resolved. Therefore, they exempt the OBJN of any participation whatsoever in any imbroglios concerning the content under consideration. All authors declare that they have no conflict of interest of financial or personal nature concerning this manuscript which may influence the writing and/or interpretation of the findings. This statement has been digitally signed by all authors as recommended by the ICMJE, whose model is available in http://www.objnursing.uff.br/normas/DUDE_eng_13-06-2013.pdf
Received: 11/29/2015 Revised: 07/19/2016 Approved: 07/24/2016